Chapters
Part VIII: Other issues
8.1 Management of penicillin allergy
8.1.1 Background
- Studies have shown that 70–90% of patients who gave a history of penicillin allergy could actually tolerate penicillin.
- It has been estimated that less than 15% of patients with penicillin allergy are still allergic ten years after their last reaction.
- There is extensive cross-reactivity between drugs in the penicillin family. Patients who are allergic to one penicillin drug must therefore avoid other members of the family.
- On the other hand, unnecessary avoidance of penicillin in patients who are not actually allergic would result in extra cost and overuse of drugs that should be reserved for treating drug-resistant organisms, such as vancomycin.
- Certain penicillin drugs are commonly associated with drug rashes. These reactions, although usually mild, can nevertheless result in patient dissatisfaction.
- Skin testing with major and minor determinants of penicillin, together with benzylpenicillin and amoxicillin, as well as other suspected ß-lactams, can reliably rule out IgE-mediated penicillin allergy.
- Patients with IgE-mediated ß-lactam allergy can be successfully desensitised just prior to starting treatment.
8.1.2 Dealing with patients with a remote history of penicillin allergy
- Determine the date of the last reaction, the type of reaction, the timing of the reaction and other extenuating circumstances, such as infectious mononucleosis and other infections (Figure 8.1).
- Patients who give a history consistent with severe drug allergy, including Stevens-Johnson syndrome, toxic epidermal necrolysis and drug hypersensitivity syndrome must not be given drugs from the same family again.
- Patients who give a history consistent with an IgE-mediated reaction (urticaria, angioedema, anaphylaxis) should use an alternative agent (see 8.1.5 below). If penicillin is strongly indicated, skin testing can be performed to assess the risk of anaphylaxis (Figure 8.2). If skin testing is not available, rapid oral desensitisation can be performed (Table 8.1) with informed consent just prior to drug administration.
- Serum specific IgE tests of ß-lactam drugs have such a low sensitivity that they only have a complementary role.
- Basophil activation tests have a better sensitivity but they are not yet available for clinical service in HK (512).
- In patients who give a history of minor drug rash, penicillin is not absolutely contraindicated. However, the physician should first consider using an alternative agent to avoid patient dissatisfaction. Under circumstances where the use of penicillin is clinically desirable, the treating physician should carefully explain the rationale and obtain the patient's informed consent. This should be recorded in the patient's medical record. It is also prudent to give a test dose of 1/10th of the treatment dose first and observed for one hour, as the history might not be completely reliable in excluding IgE-mediated reactions.
8.1.3 Dealing with patients with a definite history of IgE-mediated penicillin allergy
- Patient who had reactions that were medically verified as IgE-mediated should use an alternative agent.
- If penicillin is strongly indicated, desensitisation should be carried out with informed consent just prior to drug administration.
8.1.4 Dealing with patients with a history of cephalosporin allergy
- Cephalosporins generally have a much lower risk of allergic reactions compared to penicillin because their ß-lactam ring is rapidly broken down in vivo.
- Cross-reactivity tends to occur between cephalosporins with similar side chains. It is therefore possible to substitute a cephalosporin with side-chains different from that of the offending drug (Table 8.2).
- Since cephalosporin allergy is due to side-chain reactivity, skin testing with the classic penicillin agents, together with the native drug can reliably predict the likelihood of IgE-mediated reactions.
- Therefore, if the patient is allergic to a clearly identified cephalosporin and no satisfactory alternative is available, the physician can choose another cephalosporin with different side-chains. Skin testing should be performed with the classic pencillin agents and the drug to rule out the risk of IgE-mediated reaction. The drug can then be administered after obtaining the patient's informed consent.
8.1.5 Choosing an alternative drug for patients with ß-lactam allergy
- As cephalosporins have a spectrum of antimicrobial activity similar to penicillin, they are actually good alternatives for patients with penicillin allergy.
- Unfortunately, product inserts often list penicillin allergy as a contraindication to the use of cephalosporins. This information was based on early experiences with first generation cephalosporins and is no longer up to date. However, there are medico-legal implications when using cephalosporins in patients with penicillin allergy.
- Second, third and fourth generation cephalosporins have negligible cross-reactivity with penicillin and are good alternatives, as long as one chooses agents that do not share similar side-chains with penicillin G, ampicillin or amoxicillin (Table 8.2). These drugs should be given by graded challenge after a negative skin test with this cephalosporin.
- Patients with penicillin allergy have a higher risk of becoming allergic to any drug in general. This fact should be communicated to the patient and the rationale for using the alternative agent explained. Informed consent should be obtained and recorded in the medical record.
- Carbapenems can also be safely used in patients with penicillin and cephalosporin allergy if clinically indicated.
- Macrolides, fluoroquinolones, lincomycins and aminoglycosides do not cross-react with ß-lactams.
- Vancomycin should only be considered as a substitute if clinical circumstances dictate its use, i.e. MRSA, Enterococcus, etc..
Table 8.1 Oral ß-lactam desensitisation protocol1
| Dose | Concentration (mg/mL) | Volume (mL) | Time | Reaction |
|---|---|---|---|---|
| 1 | 0.1 | 0.3 | 0:00 | |
| 2 | 0.1 | 0.6 | 0:15 | |
| 3 | 0.1 | 1.2 | 0:30 | |
| 4 | 0.1 | 2.5 | 0:45 | |
| 5 | 0.1 | 5 | 1:00 | |
| 6 | 1 | 1 | 1:15 | |
| 7 | 1 | 2 | 1:30 | |
| 8 | 1 | 4 | 1:45 | |
| 9 | 10 | 0.8 | 2:00 | |
| 10 | 10 | 1.6 | 2:15 | |
| 11 | 10 | 3.2 | 2:30 | |
| 12 | 10 | 6.4 | 2:45 | |
| 13 | 100 | 1.2 | 3:00 | |
| 14 | 100 | 2.5 | 3:15 |
- Prepare stock solution of ß-lactam drug that you wish to use at 100 mg/mL.
- Make serial dilutions at 10 mg/mL, 1 mg/mL, 0.1 mg/mL.
- Administer doses at 15-minute intervals.
- Have epinephrine 1:1,000 on stand-by at bedside.
- Once successfully desensitised, begin treatment immediately.
- To maintain desensitised state, patient must not interrupt treatment for more than 2 days. Otherwise, patient would need to be desensitised again.
Note:
1Reference: (513)
Table 8.2 Cross-reacting side chains between ß-lactam antibiotics
| Amoxicillin | Ampicillin | Cefaclor | Cefadroxil | Cefepime | Cefoperazone | Cefotaxime | Cefoxitin | Cefpodoxime | Ceftazidime | Ceftibuten | Ceftriaxone | Cefuroxime | Cephalexin | Cephaloridine | Cephalothin | Cephradine | Penicillin G | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Amoxicillin | 6 | 6/7 | 6/7 | 6/7 | 6/7 | |||||||||||||
| Ampicillin | 6 | 6/7 | 6/7 | 6/7 | 6/7 | |||||||||||||
| Cefaclor | 6/7 | 6/7 | 7 | 7 | 7 | |||||||||||||
| Cefadroxil | 6/7 | 6/7 | 7 | 3,7 | 3,7 | |||||||||||||
| Cefepime | 7 | 7 | 7 | |||||||||||||||
| Cefoperazone | ||||||||||||||||||
| Cefotaxime | 7 | 7 | 7 | 3 | ||||||||||||||
| Cefoxitin | 3 | 7 | 7 | 6/7 | ||||||||||||||
| Cefpodoxime | 7 | 7 | 7 | |||||||||||||||
| Ceftazidime | ||||||||||||||||||
| Ceftibuten | ||||||||||||||||||
| Ceftriaxone | 7 | 7 | 7 | |||||||||||||||
| Cefuroxime | 3 | |||||||||||||||||
| Cephalexin | 6/7 | 6/7 | 7 | 3,7 | 3,7 | |||||||||||||
| Cephaloridine | 7 | 7 | 6/7 | |||||||||||||||
| Cephalothin | 3 | 7 | 7 | 6/7 | ||||||||||||||
| Cephradine | 6/7 | 6/7 | 7 | 3,7 | 3,7 | |||||||||||||
| Penicillin G | 6/7 | 6/7 | 6/7 |
Numbers denote position of side chains: 3, similarity at the cephalosporin 3—position side chain; 7, similarity at the cephalosporin 7—position side chain; 6/7, similarity at the penicillin 6—position side chain and the cephalosporin 7—position side chain.
Each number in the matrix indicates side-chain similarity between two drugs. Cross-allergenicity is expected between each similar pair. For example, a patient allergic to amoxicillin would very likely manifest an allergic reaction to ampicillin, cefadroxil, cefaclor, cephalexin and cephradine. However, the patient would not be expected to exhibit an allergic response to cefepime, cefoperazone, cefotaxime, etc., unless he/she was also allergic to another cephalosporin or penicillin with a similar side chain to the reference drug.
Reference: (514)
Table 8.3 Risk of cross-reactivity between different ß-lactams
| Allergic to | Drug of concern | Risk of cross-reactivity |
|---|---|---|
| Cephalosporin | Penicillin | 8.3%–25.5% in two series (515–516) *Cephalosporins with structures similar or identical to penicillin have 3-fold increase in risk |
| Carbapenems | Imipenem 2% and meropenem 1% in one series | |
| Penicillin | Cephalosporins | 10.9% with most involving cephalothin and cefamandole (517) |
| Carbapenems | Meropenem 0.9%, imipenem 0.9% (518–520) | |
| All first generation cephalosporins | Odds ratio: first generation cephalosporins 4.2, second generation cephalosporins 1.1 and third generation cephalosporins 0.8 (521) | |
| Cephalexin | 31% in one series with 16 patients (522) | |
| Amoxicillin | Cefadroxil | 38% (cefadroxil has identical side chain to amoxicillin) (523) |
| Cefamandole | 0% for 21 patients (different side chain to amoxicillin) (523) |
Figure 8.1 Flow chart on assessment of ß-lactam allergy
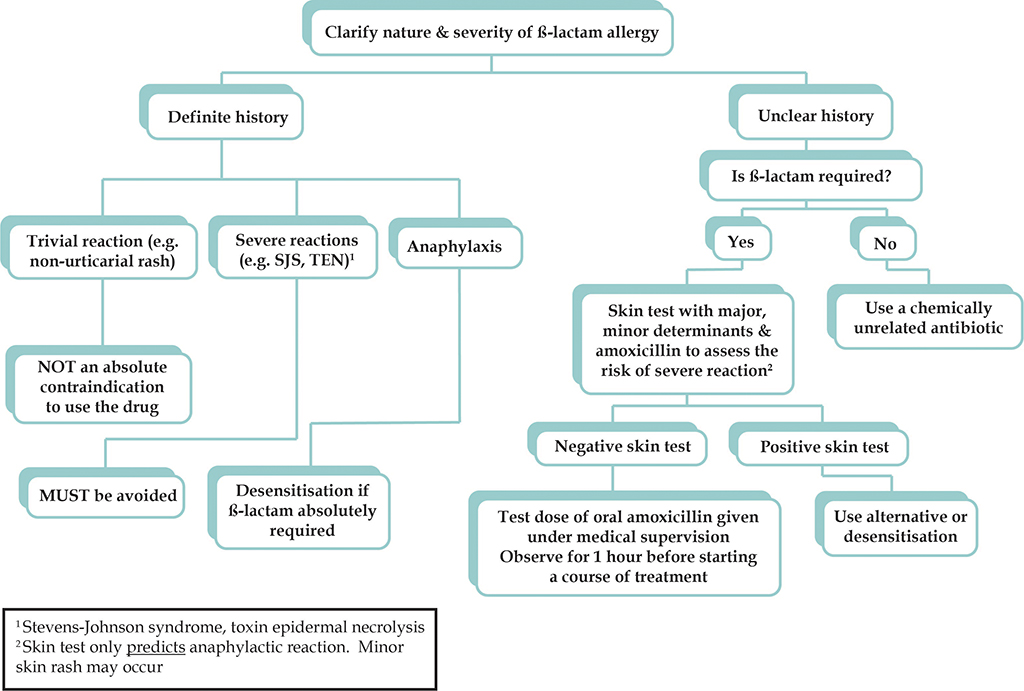
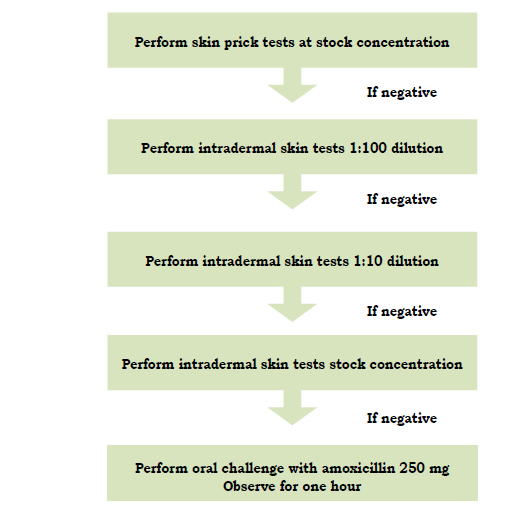
Figure 8.2 ß-lactam skin testing
Stock test solutions:
- Peniclloyl polylysine (PPL) 0.04 mg/mL
- Minor determinant mix (MDM) 0.5 mg/mL
- Ampicillin 20 mg/mL
- Ampicillin 20 mg/mL
- Cephalosporins 20 mg/mL
Note that all stock concentrations are in mg/mL
Precautions
This should only be conducted by persons with the proper training.
Have epinephrine 1:1,000
on stand-by when performing skin tests.
Procedure