Home > Chapters
Chapters
Part IV: Recommendation for the empirical therapy of common infections
4.2 Guidelines on the use and choice of antibiotics in severe acute pancreatitis (SAP)
- Criteria for severity assessment of acute pancreatitis (Table 4.2)
Most acute pancreatitis is mild. SAP occurs in about 5–13% of all patients with mortality rates of 30% (337–341). SAP is currently defined as having persistent (>48h) single or multiple organ failure as a result of acute pancreatitis, which is most often associated with local (such as peri-pancreatic collections) and/or systemic complications. Patients diagnosed to have SAP are advised to be transferred for close monitoring and treatment in an ICU. Numerous clinical and laboratory findings have been shown to be associated with severe disease course in acute pancreatitis. A number of well-known scoring systems have been employed to predict disease severity at or shortly after admission, though none of which is clearly superior in performance: (a) Ranson score (≥3); (b) persistent systemic inflammatory response syndrome >48h (Table 4.2); (c) bedside index for severity in acute pancreatitis score (≥3); and acute physiology and chronic health evaluation II (APACHE II) criteria (>8) (340,342–346). A C-reactive protein value of ≥150μg/mL has also been shown to be useful in predicting the severity of acute pancreatitis (347). - Routine antibiotic prophylaxis not beneficial
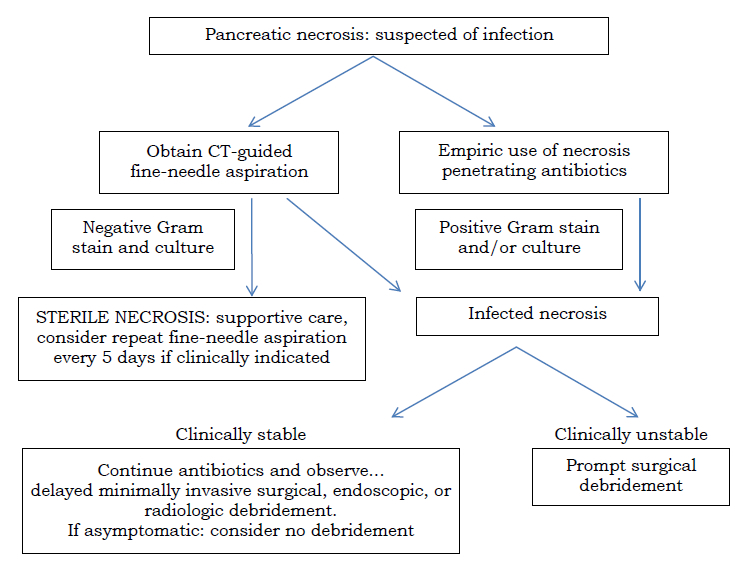
Despite previous uncertainty over this issue due to conflicting evidence in the literature (348–356), the current consensus is that prophylactic use of antibiotics in acute pancreatitis is not advisable (343–346,357–361). Documented drawbacks of prophylactic antibiotics included selection of multidrug-resistant organisms (MRSA, CRAB, resistant Enterobacteriaceae), increased Candida infections, and antibiotic-related adverse event which may lead to poorer patient outcomes (337,362–370). Therefore, broad-spectrum antibiotics should only be used when clinical factors point to infected pancreatic necrosis (greatest risk in those with >30% pancreatic necrosis) (371). - Management of pancreatic necrosis when infection is suspected (Figure 4.1) (340-341,343–346,360–361)
Infected necrosis should be considered in patients with pancreatic or extrapancreatic necrosis who deteriorate or fail to improve after 7–10 days of hospitalisation. The finding on computerised tomography of gas within a collection or necrotic area is considered strong evidence of infection. When infected necrosis is suspected, computerised tomography or ultrasound guided-fine-needle aspiration of necrotic area for culture can be performed, or empirical antibiotics with good penetration into pancreatic tissue and providing broad coverage against enteric Gram-negatives bacilli and anaerobes may be given (e.g. an I.V. carbapenem) (338–339,372–373). Although unstable patients with infected necrosis should undergo urgent debridement, current consensus is that the initial management of infected necrosis for patients who are clinically stable should be a course of antibiotics before intervention to allow the inflammatory reaction to become better organised. If the patient remains ill and the infected necrosis has not resolved, minimally invasive necrosectomy by endoscopic, radiologic, video-assisted retroperitoneal, laparoscopic approach, or combination thereof, or open surgery is recommended once the necrosis is walled-off.
Table 4.2 Severity grading of acute pancreatitis according to revised Atlanta criteria (2012) (374)
| Mild acute pancreatitis |
|---|
| No organ failure No local or systemic complications |
| Moderately severe acute pancreatitis |
| Organ failure that resolves within 48 h (transient organ failure) and/or Local or systemic complications without persistent organ failure |
| Severe acute pancreatitis |
Persistent organ failure (>48 h)
|
Figure 4.1 Management of pancreatic necrosis when infection is suspected (343)